The Science Behind Our Products
Our patented formula, used to develop both Pre Lubricant and Preseed Intimate Moisturizer, is unique. Traditional lubricants have been developed to decrease friction or pain during sexual intercourse. Their basic formulations can harm sperm within minutes of contact. Preseed is the only intimate moisturizer formulated by an Andrologist, based on the physiologic requirements of sperm, so as to provide an environment that will not harm them. A quick review of our ingredients shows how our formula is unique, in using components that provide moisture, but also that ensures sperm encounter an optimal environment. This includes arabinogalactan for antioxidant support. Our formulas do also contain very low concentrations of parabens as a preservative. We are aware this has caused concern for some; however, the paraben level in our products is 25% of the minimum concentration found to interfere with sperm function in the extreme condition of direct culture in vitro (Song et al., 1989), as previously reported. Based on the IVF and embryo development studies done by Dr.Wright (using a robust bovine model) it is clear that even 50% direct contact of our formula with gametes did not interfere with fertilization or embryo development. This data assured us that the paraben level in our products is appropriate as a preservative for user protection, without harming gamete function.
Over the past decade there have been many presentations at medical meetings and some full publications on our technology, from both in house and third party investigators. These include those having to do with the beneficial role of arabinogalactan on sperm cell function, primarily through mitigation of oxidative stress damage to motility and chromatin integrity.
We are proud of the many studies we have done to confirm the unique nature of our products. These studies have allowed Pre Lubricant to be the first ever with specific indications of use including fertility interventions. Such uses include:
| |
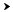 Semen collection using polyurethane condoms Semen collection using polyurethane condoms
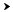 Embryo transfer Embryo transfer
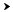 Transvaginal collection of oocytes Transvaginal collection of oocytes
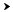 Intrauterine insemination Intrauterine insemination
 Post coital testing Post coital testing |
If you have any questions regarding this science please feel free to contact us at info@inhealth.ie
Full Publications on Products
We are very pleased to have access to the following full publications, written by independent third parties about our product line:
Effect of Vaginal Lubricants on Sperm Motility and Chromatin Integrity: A Prospective Comparative Study
Fertility & Sterility, 2008 Feb;89(2):375-379
Agarwal A, Deepinder F, Cocuzza M, Short RA, Evenson DP. Reproductive Research Center, Glickman Urological Institute and Department of Obstetrics-Gynecology, Cleveland Clinic, Cleveland, Ohio.
Objective: To evaluate the effect of vaginal lubricants Pre~Seed, FemGlide, Astroglide, and Replens on human sperm motility and chromatin integrity.
Design: Prospective, comparative, in vitro study.
Setting: Andrology laboratory at tertiary care hospital.
Patient(s): Thirteen normozoospermic donors.
Intervention(s): Semen samples from 13 subjects were incubated in human tubal fluid media (HTF) controls and 10% (vol/vol) of Pre seed, FemGlide, Astroglide, and Replens lubricants. After 30 minutes, progressive sperm motility was assessed by light microscopy. Semen samples of 12 patients were placed in positive control (HTF), negative control (10% K-Y Jelly lubricant), and 10% vol/vol Pre~Seed and FemGlide lubricants. After 4 hours culture, spermatozoa were analyzed for percent DNA fragmentation index with use of the acridine orange-based sperm chromatin structure assay.
Main Outcome Measure(s): Sperm motility and percent DNA fragmentation index.
Results: Percent motility did not differ significantly between HTF controls and Pre~Seed, whereas FemGlide, Replens, and Astroglide lubricants demonstrated a significant decrease in motility. There was no significant difference in percent DNA fragmentation index between the HTF controls and Pre~Seed, but a significant decline in sperm chromatin quality occurred with FemGlide and K-Y Jelly.
Conclusion: Pre seed does not cause a significant decrease in progressive sperm motility or chromatin integrity in contrast to other lubricants used by couples.
Irritation Potential of Personal Lubricants Relates to Product Osmolality as Detected by the SMI (Slug Mucosal Irritation Assay)
Sexually Transmitted Diseases, 2008 May;35(5):512-516
Els ADRIAENS, PhD; Jean Paul REMON, PharmD. Laboratory of Pharmaceutical Technology, Ghent University, Harelbekestraat 72, 9000 Ghent, Belgium
BACKGROUND: The slug mucosal irritation assay has recently been used as a sensitive measure of mucus membrane tolerance for vaginal microbicide products and carriers. In the current study, it was determined whether musosal irritation potency of personal lubricants is related to varying product osmolalities.
METHODS: Five commercial lubricants with an osmolality range were evaluated using the previously validated slug mucosal irritation assay. Specifically, Arion lusitanicus were treated with lubricants over 5 days to quantify mucus production and tissue damage, allowing assignment of each product into an irritation potency category (none, mild, moderate, or severe).
RESULTS: The irritation potency (assessed by the mucus production) of the lubricants showed a significant, quadratic relationship with the product osmolality (P = 0.001; R (2) = 0.99). Femglide, a hypo-osmotic lubricant (32 mOsm/kg), caused a negative mucus production. Pre, an iso-osmotic lubricant (316 mOsm/kg), caused no changes. Two moderately hyperosmotic lubricants, Replens and K-Y jelly (2143 and 2463 mOsm/kg), induced mild and moderate irritation, respectively. The highly hyperosmotic lubricant Astroglide (5848 mOsm/kg) resulted in severe irritation and tissue damage.
CONCLUSIONS: Commonly used personal lubricants show a full range of mucosal irritation potential, which is related to product osmolality. Toxicity Tests Carried Out On the PRE-SEED Lubricant Compared With Other Commercially Available Brands (FELIS, REPLENS, AQUASONIC)
In Preparation for Submission to Human Reproduction, 2007
Josefina Vargas, Dr Alfred Senn , Prof. Marc Germond. Fondation Faber, Lausanne Switzerland
Several studies have shown that gels used to treat vaginal dryness are liable to affect the motility, chromatin integrity and kinetic parameters of human spermatozoids to varying degrees. The chemical-physical elements that play a role in the mechanism for reducing motility are principally a drop in pH and a change in ionic strength. In our study, we compared different commercially available lubricants (Felis, Replens and Pre-Seed) with a gel routinely used by gynecologists during vaginal US (Aquasonic). Several concentrations of these products were tested in an HTF medium to which albumin was added (10% SSS), and were also subject to two periods of exposure (1 hr and 24 hrs). In order that all of the solutions tested should be subject to identical handling, we selected the weakest C1 concentration (0.083%) as the control. Taken together, these conditions allow the motility of spermatozoids to be maintained in the controls for 24 hours at values close to those at time 0. In our study, Replens lubricant and the Aquasonic US gel have a negative effect on the motility of spermatozoids even at the weakest concentrations (C2, C3 and C4). The Felis lubricant, in contrast, exercises a negative action at higher concentrations, i.e. C3 and C4. Pre-Seed, on the other hand, has no negative effect on the survival of spermatozoids at any of the concentrations tested. In conclusion, of all of the gels and lubricants tested, Pre-Seed appears to guarantee optimal conditions for the survival of spermatozoids in vitro and can be recommended by gynecologists to infertile patients suffering from vaginal dryness. The negative role of the gels used for vaginal US poses a significant problem, because these are regularly used for echographs to monitor ovarian stimulation in infertile patients.
Medical Meetings
Studies on INGfertility Technology Presented at Major Medical Meetings
Animal Model Study of a New Patient Lubricant's Affect on In Vitro Fertilization & Embryo Development
American Society of Andrology Annual Meeting, Orlando FL, April 2007 ( RW Wright Jr, Center for Reproductive Biology, WSU Pullman, WA )
Experiments were done to evaluate in vitro fertilization and embryo development following sperm exposure to products used to lubricate devices in fertility medicine including: KY® Gel, Aquasonic® Ultrasound Gel and Pre (a new Patient Lubricant recently cleared for use during fertility interventions). Bovine in vitro fertilization and embryo culture methods are standard and have been proposed as an excellent model for gamete toxicity studies (ReprodBioMed Online 2002;4:170-5). In this study, cryopreserved bull sperm (from a single bull) were routinely washed, resuspended in a TALP medium and placed into one of 5 treatments. These included: 1) Control sperm in medium alone; or sperm medium suspensions with the following added (v/v) 2) 10% Pre’ lubricant; 3) 50% Pre’ lubricant; 4) 10% KY®; or 5) 10% Aquasonic® Gel. Sperm were incubated in treatments for 30 min at body temperature, and placed into fertilization wells with mature oocytes (1 x 106 sperm cells per well). At 8 hrs, putative zygotes were transferred into embryo culture medium and further incubated. At 32 hr of culture, dividing embryos were counted (% fertilization in each treatment). Final development rates were evaluated on Day 7 (post IVF) to determine the % of total oocytes that had developed to the morula or blastocyst stage. ANOVA was used to compare the % fertilization of oocytes & the % of normal embryo development resulting from sperm in each treatment (as seen in Table below, data are mean +/- sd).
In Vitro Fertilization & Embryo Development After Sperm Exposure
|
|
% Fertilized Oocytes (+ sd)
|
% Embryos Developing (+ sd) |
| Control Medium |
80 |
61(5)a |
40(9)a |
| Pre’ 10% |
80 |
60(8)a |
39(8)a |
| Pre’ 50% |
80 |
59(6)b |
43(10)b |
| KY 10% |
80 |
0c |
0c |
Aquasonic10% |
80 |
0c |
0c |
|
a,b,c denote means that differ within column by p<0.0001(ANOVA).
Pre’ Patient Lubricant did not interfere with the ability of sperm to fertilize oocytes or support embryo development in vitro (using a bovine model) even at high concentrations. Conversely, KY® and Aquasonic® significantly impacted the ability of sperm to fertilize oocytes, and allow normal embryo development.
Changes in Sperm Motility and Chromatin Integrity Following Contact with Vaginal Lubricants American Society of Reproductive Medicine Annual Meeting, Montreal Quebec, October 2005 (now a full publication in Fertility & Sterility, 2007: Effect of vaginal lubricants on sperm motility and chromatin integrity: a prospective comparative study).
Agarwal A, Deepinder F, Cocuzza M, Short RA, Evenson DP.
Reproductive Research Center, Glickman Urological Institute and Department of Obstetrics-Gynecology, Cleveland Clinic, Cleveland, Ohio.
OBJECTIVE: To evaluate the effect of vaginal lubricants Pre-Seed®, FemGlide®, Astroglide®, and Replens® on human sperm motility and chromatin integrity. DESIGN: Prospective, comparative, in vitro study. SETTING: Andrology laboratory at tertiary care hospital. PATIENT(S): Thirteen normozoospermic donors. INTERVENTION(S): Semen samples from 13 subjects were incubated in human tubal fluid media (HTF) controls and 10% (vol/vol) of Pre-Seed®, FemGlide®, Astroglide®, and Replens® lubricants. After 30 minutes, progressive sperm motility was assessed by light microscopy. Semen samples of 12 patients were placed in positive control (HTF), negative control (10% K-Y Jelly® lubricant), and 10% vol/vol Pre-Seed® and FemGlide® lubricants. After 4 hours culture, spermatozoa were analyzed for percent DNA fragmentation index with use of the acridine orange-based sperm chromatin structure assay. MAIN OUTCOME MEASURE(S): Sperm motility and percent DNA fragmentation index. RESULTS: Percent motility did not differ significantly between HTF controls and Pre-Seed®, whereas FemGlide®, Replens®, and Astroglide® lubricants demonstrated a significant decrease in motility. There was no significant difference in percent DNA fragmentation index between the HTF controls and Pre-Seed®, but a significant decline in sperm chromatin quality occurred with FemGlide® and K-Y Jelly®.
CONCLUSION: Pre-Seed does not cause a significant decrease in progressive sperm motility or chromatin integrity in contrast to other lubricants used by couples.
The Effects of Vaginal Lubricants and Moisturizers on Computer Assisted Sperm Analysis (CASA) Parameters Associated with Cervical Mucus Penetration
American Society of Reproductive Medicine Annual Meeting, Philadelphia PA, October 2004
JE Ellington, and J. Schimmels, INGfertility, Spokane, WA and Washington State University, Spokane, WA
Objective: The incidence of vaginal dryness is increased in trying to conceive (TTC) couples; however, numerous papers have cited the detrimental effect of common vaginal lubricants and moisturizers on sperm motility. To date, studies have not been done using CASA to evaluate the effects of lubricant products on the motion characteristics of sperm thought to be associated with cervical mucus transport. Specifically, samples of sperm with mean average path velocity (VAP), % straightness (STR) and Amplitude of Lateral Head Displacement (ALH) exceeding a predetermined level have recently been proposed to have a superior likelihood of good cervical mucus penetration in vivo. Numerous studies have found a correlation between such ability of sperm to penetrate cervical mucus and pregnancy outcomes. The current study evaluated sperm motion parameters following contact with several vaginal lubricants/moisturizers, to determine their impact on CASA outcomes associated with good cervical mucus penetration, as well as overall motility.
Design: Prospective, comparative, in-vitro study.
Materials and Methods: Raw semen from 25 normospermic donors was diluted 1:1 with Human Tubal Fluid. Each sample was then divided into one ml aliquots and placed into multiple culture wells. Vaginal lubricants/moisturizers as shown in the Table below were applied across these wells to achieve a final 10% v/v concentration, and incubated at 37oC for 30 min. CASA of sperm from these treatments and those in a control well (with no lubricant) was then performed. Samples in each treatment fulfilling all of the following parameters were given a positive penetration score (e.g. likely to penetrate cervical mucus well): VAP > 25 micron/sec; STR >80%; and ALH >2.5 microns. Positive penetration scores were reported as a percent of all samples tested and compared between the treatments. Additionally, mean outcomes in each treatment were determined and compared for the individual CASA parameters, as well as for the overall percentage of motile sperm.
Results: The mean motion characteristics for these specific CASA criteria (+/- SEM) and percent samples with a positive penetration score are shown in the Table below. Means with differing superscripts differ from the control at p<0.05.
| Sperm Motility Following Contact with Vaginal Lubricants. |
Treatment |
|
|
ALH |
Overall % Motile |
%Samples w/ + Score |
| Control Media |
56 +/-3 |
81 +/-2 |
3.9 +/-0.3 |
70 +/-4 |
61b |
| FemGlide |
50 +/-2 |
81 +/-4 |
3.7 +/-0.4 |
61 +/-3 |
68b |
| Pre~Seed |
53 +/-3 |
85 +/-3 |
3.6 +/-0.2 |
76 +/-3 |
90a |
| KY Jelly |
49 +/-4 |
80 +/-4 |
2.4 +/-0.6a |
29a +/-2 |
20c |
| Astroglide |
39a +/-3 |
74 +/-3 |
2.6 +/-0.5a |
5a +/-0.4 |
10c |
| Replens |
* |
* |
* |
15a +/-2 |
* |
|
Replens caused the media to abruptly turn very acidic and opaque. Further, sperm clumping occurred to the point that meaningful CASA data could not be generated.
Conclusion: Within 30 minutes of exposure, a 10% v/v concentration of the most commonly used lubricant products significantly decreased sperm motility and penetration scores. The percentage of samples with a positive penetration score was significantly improved with Preseed as compared to the other treatments. Products used to alleviate vaginal dryness that negatively effect sperm motility and transport should be avoided by TTC couples. Studies to determine the in vivo impact of vaginal lubricants/moisturizers on cervical mucus penetration are ongoing.
Support: NICHD SBIR to INGfertility.
Prevalence of vaginal dryness in trying to conceive couples
Pacific Coast Reproductive Society Annual Meeting, Rancho Mirage CA, April 2003
JE Ellington, and RA Short INGfertility, Spokane, WA & Washington State University, Spokane, WA
Dyspareunia, primarily due to vaginal dryness, has been reported to occur “sometimes” or “more often”, in at least 46% of all reproductive age women. However, it is currently not known if vaginal dryness is increased in trying-to-conceive (TTC) couples. Additionally, it is not known how TTC couples are managing symptoms of vaginal dryness, given numerous reports on the sperm-toxic nature of most personal lubricants and even saliva.This study was done to determine the prevalence of vaginal dryness among TTC couples, and their level of understanding of appropriate interventions for such dryness. An opt-in internet survey of 900 TTC couples was conducted over 5 months. Thirty questions regarding fertility and vaginal dryness were asked of each participant. Summary statistics for the group were compiled and analyzed.
Average TTC time for the group was 7 months, with 33% TTC 1 year or more. Medical care for their fertility issues included: 23% no doctor, 13% PCP, 43% ObGyn, 16% Fertility Specialist, 4% Urologist. Most couples (78%) had no definitive diagnosis for cause of fertility problems. Most (69%) routinely used some ovulation prediction method. Only 16% were currently taking “fertility medications”.
While TTC, vaginal dryness negatively affected sexual intimacy for most couples: 11% always, 35% often, 42% sometimes, 9% rarely, 3% never. Vaginal dryness episodes also increased while TTC: 19% a lot, 57% some, 23% not at all. Although 30% knew not to use a lubricant while TTC, another 26% often or always used such products. Use by this later group included mostly that of KY® (40%) and Astroglide® (19%). Only 20% of couples had ever discussed their dryness problem with a doctor. Of those that had, 75% of the doctors reiterated the sperm-toxic effects of lubricants.
Rates of vaginal dryness in TTC couples appears to be as much as twice that seen in the general population. Patients are not discussing this problem with their care providers adequately. Fully one-quarter of TTC couples are utilizing personal lubricant products which reportedly are as toxic to sperm as are contraceptive jellies. Products designed specifically to relieve vaginal dryness without harming sperm, such as Pre~Seed, are needed for use by TTC couples.
Effects of Personal Lubricants on In Vitro Fertilization and Embryo Development
American Society of Andrology Annual Meeting, Phoenix AZ, March 2003
RW Wright1, PhD; RA Short2, PhD; & JE Ellington3 DVM, PhD 1Dept Animal Science & 2Health Research Center, Washington State University; and 3INGfertility, Spokane, WA
Use of personal lubricants is not recommended for couples that are trying to conceive based on several studies reporting their deleterious effect on sperm motility. In spite of this, 43% of all trying-to-conceive couples use personal lubricant products due to a high frequency of vaginal dryness. The current study was designed to compare in vitro fertilization and embryo development of bovine oocytes in the presence of moderate doses (10%) of several different products. In vitro matured cow oocytes were fertilized by bull sperm with: 10% KY Jelly®; 10% FemGlide® (labeled as "sperm compatible"); 10% Pre seed (a new moisturizer developed to provide an optimal sperm environment); and control TALP IVF media. Lubricants were only present during the fertilization incubation of sperm and oocytes. The bovine IVF model allows for detection of sperm DNA damage which can inhibit embryo development. Embryos were cultured for 7 days and then scored for normal development for blastocyst (multi-cell) stage. Data are expressed as Mean(SEM).Treatment
|
|
|
% Blasts |
| KY Jelly |
100 |
12 (2.0)a |
2 (1.2)a |
| FemGlide |
200 |
72 (3.4)b |
42 (0.7)b |
| Pre~Seed |
200 |
73 (4.6)b |
47 (0.9)c |
| Control |
200 |
77 ( 3.4)b |
44 (0.8)b,c |
|
KY Jelly in the fertilization medium had a very negative effect on fertilization and development (a,c differ by p<0.001), with only 2% of all eggs developing to the blastocyst stage. FemGlide decreased embryo development as compared to the Pre seed® treated sperm (b,c differ by p=0.05). Pre seed did not effect embryo development as compared to the control media in this model, in fact a trend for improved development was seen. Mouse embryo development studies with 10% volume of test product are routinely done as a toxicology screen for assisted reproduction media. A similar design, using cow embryos detected a harmful effect of KY Jelly and FemGlide on embryo development after sperm exposure to these products.
Effect of New Intimate Moisturizer on Sperm Motility
American Society of Andrology Annual Meeting, Phoenix AZ, March 2003
JE Ellington1 PhD; RA Short2 PhD; & J Schimmels1 1INGfertility, Spokane, WA & 2Health Research Center, Washington State University, Spokane, WA
Numerous publications cite the deleterious effect of existing commercial lubricants on sperm motility. Additionally, 75% of trying-to-conceive couples have an increased incidence of vaginal dryness. This study compared motility parameters for human sperm (n=25 ejaculates) cultured for 30 min in HTF media with HSA (control), to which either 10% KY Jelly®; 10% Astroglide®; 10% FemGlide® (marketed as “sperm compatible”); or 10% Pre seed® (specifically developed to not harm sperm) were added.
|
|
|
VCL
(µm/s) |
|
| Control Media |
100a |
53 (2)a |
89 (3)a |
59 (2)a |
| KY Jelly |
62 (6)b |
37 (2)b |
67 (2)b |
40 (2)b |
| FemGlide |
92 (4)c |
44 (4)c |
79 (3)c |
50 (4)c |
| Pre seed |
100 (5)a |
51 (2)a |
79 (2)c |
56 (3)a,c |
| Astroglide |
<5 |
NA |
NA |
NA |
|
a,b,c Superscripts show means (SEM) within a column that differ at p<0.05.
Due in part to viscosity change, all lubricants slowed sperm velocity as compared to control medium. However, sperm in Pre-Seed retained motility equivalent to the control over the 30 min of culture, whereas sperm in the other lubricants had decreased motility (p<0.05). This effect was profound with Astroglide. Placed side by side, FemGlide and KY created a distinct barrier whereby sperm in raw semen had difficulty penetrating into the products (photos available). In contrast, sperm moved freely between raw semen and the Pre~Seed.
Polysaccharides Containing Arabinose and Galactose Decrease Oxidative Damage to Sperm In Vitro
American Society of Andrology Annual Meeting, Montreal Quebec, June 2002
JE Ellington, SA Oliver, DP Evenson Washington State University, Spokane, WA and South Dakota State University, Brookings, SD
Polysaccharides containing arabinose & galactose (PCAG), such as arabinogalactan, are abundant in plant gums. These PCAG have a membrane stabilizing effect in a variety of cell types. Studies were done to determine the effects of PCAG on bull sperm during freezing and culture.
In Experiment 1: ejaculates from 4 bulls at a commercial AI stud were frozen in standard egg yolk buffer (EYB) or in egg yolk buffer with PCAG (PEYB). Six straws of sperm from each bull and treatment were thawed and: 1) held at 37° C for 10 min, then evaluated for membrane lipid peroxidation (TBARS assay) and sperm chromatin damage (Sperm Chromatin Structure Assay); or 2) cultured in routine TALP medium for 24h to determine sperm survival rates.
Results: sperm frozen in EYB had more oxidative (p=0.03) and chromatin (p=0.01) damage after thawing than sperm in PEYB. Only 1 of 4 bulls had > 10% motile sperm at 24h of culture for sperm frozen in EYB; whereas 3 of 4 bulls had >10% motile sperm for sperm frozen in PEYB.
In Experiment 2: sperm from 5 bulls (4 straws each) frozen in standard EYB were thawed, washed and placed in TALP either w/or w/o PCAG for culture at 37° C. At 4h, sperm motility was determined and aliquots were removed to determine membrane lipid peroxidation.
Results: More sperm were motile (p=0.04) and had lower oxidative damage (p=0.01) in TALP with added PCAG, than in TALP alone. Follow-up studies identified an active fraction of the PCAG between 20K and 100K which promoted sperm motility and membrane stability. Preliminary studies have shown decreased oxidative stress and chromatin damage for human sperm in culture with HTF including the PCAG.
Conclusion: PCAG stabilize sperm during assisted reproduction techniques. Specifically, they appear to decrease oxidative stress and chromatin damage.
Use of a Plant Polysaccharide Gradient to Wash Bull Sperm Improves Fertilization & Embryonic Development
International Embryo Transfer Society Annual Meeting, Salt Lake City UT, Jan 1996
JE Ellington, SA Oliver, RW Wright, CS Schneider & AJ Benson INGfertility & Washington State University - Spokane, WA
Experiment 1. A continuous gradient of 22% plant polysaccharides (arabinogalactan) in a buffered salt solution (Sperm Concept-INGfertility, Spokane, WA) was compared to a standard Percoll density gradient of 45 % and 90% using frozen-thawed bull sperm (Select Sires). Studies were designed to evaluate sperm recovery and performance in a routine IVF system as determined by fertilization rates and subsequent embryonic development. Frozen sperm from 4 bulls (2 replicates each) were washed through 4 ml of Sperm Concept (SC) or gradient Percoll (P) for 30 min at 300 x g. The pellet of sperm from P was washed again in a TALP medium prior to use. No extra wash step was used in the hemocytometer. Sperm motility was also evaluated both subjectively and objectively with an HTM Analyzer. All data are expressed as the mean SEM for SC or P treated sperm, respectively. Statistical analyses were conducted using ANOVA.
Conclusions: Recovery of sperm was significantly higher (p=0.02) after SC washing than with P (72 6% vs 53 5%). SC also tended (p= 0.08) to recover more of the motile sperm than did P (88 9% vs 73 6%). Overall percent motilities were high for both groups and did not differ (p=0.18; 95 0.3 % vs 90 3%).
Experiment 2. Pooled frozen bull sperm was also washed through either SC or P as above, treated routinely with 10 IU heparin/ml and placed with total of 1100 IVM oocytes over three replicates. Oocytes were obtained from slaughtered beef heifers. Cleavage rates were determined visually on Day 3 of culture in CZB medium. Embryo quality was recorded on Day 9 of coculture on BRL cells, followed by embryo staining (Hoechst 33258) and cell counts. Embryo evaluators were blind to the sperm washing treatment utilized prior to IVF.
Conclusion: Fertilization rates for the oocytes were improved after washing sperm through SC versus P (p=0.001; 73 2% versus 53 3%). The percentage of fertile oocytes able to develop to blastocysts by Day 9 of culture was higher after washing sperm through SC versus P (p=0.009; 59 4% vs 26 5%). Overall production of blastocysts as a percentage of total oocytes introduced into the IVF system was greater after washing sperm through SC versus P (p=0.004; 43 4% vs 18 3%). Total cell counts for blastocysts formed after fertilization with either SC or P treated sperm did not differ (p=0.25; 85 2 vs 88 2).
Overall Conclusion: Washing frozen thawed bull sperm through SC appears to offer several advantages over P gradients. A pellet of highly motile sperm cells can be obtained in one centrifugation step. Sperm exposed to the arabinogalactan-containing SC wash show improved ability to fertilize oocytes and contributed to better embryonic development to the blastocyst stage.
A Novel One Step Sperm Wash Product
Pacific Coast Fertility Annual Meeting. Palm Springs CA, March 1995Â
JE Ellington, RW Wright, S Broder 1, AJ Benson, & SA Oliver INGfertility, Spokane, WA & 1 California Cryobank, Los Angeles, CA
A continuous gradient sperm wash product containing arabinogalactan, Sperm Concept (sold as IsoCare One Step) was compared against a Percoll wash in 3 experiments.
Â
Experiment 1: In Expt. 1, fresh semen from 4 men was divided and washed either in SC or 80% Percoll (P) for 30†at 300 x g. Pellets were then washed again in media alone and sperm evaluated. All data are expressed below as mean SEM for SC versus P. There was no difference in the % motility for recovered sperm (83 4% vs 83 3%), the motility of sperm cultured for 24 h (64 6% vs 75 6%) or in the numbers of sperm recovered (p=0.6). Based on animal model data showing a lack of toxicity of SC to sperm throughout the IVF process, the next 2 experiments were done on sperm removed directly from the SC pellet, without a second media wash step.Â
Experiment 2: In Expt. 2, SC was compared to bilayer P (90%:45%), to wash fresh semen from 8 men. The % normal morphology (83% 3% vs 81 1%) and motile sperm (74 6% vs 76 3%) did not differ between treatments. Both treatments improved (p<0.09) these parameters over that found for prewashed sperm morphology (72 2%) and motility (62 5%). The % of motile sperm recovered tended to be higher (p=0.1) after SC wash (93 5% vs 80 5%).Â
Experiment 3: In Expt. 3, semen from 12 men with fertility disorders was evaluated after washing in SC or P. There was no difference in motility of recovered sperm (59 12% vs 60 16%); however, normal membrane function (hypo-osmotic swell test) was better (p=0.045) in SC (70 13% vs 46 10%). Hamster egg SPA was also done on sperm washed from 4 donors in both SC and P. There was no difference in % eggs penetrated (41 2% vs 40 2%) or in the penetration factor (0.48 0.02 vs 0.41 0.03). One man did show a 30% improvement using SC versus P. The SC product is made from a polysaccharide approved for human consumption. It offers a non-toxic one step wash alternative to Percoll. |